When patients think about a hair transplant, most focus on the front hairline or the bald crown. However, the true foundation of every successful procedure is the hair transplant donor area. Without a strong, properly managed donor region, even the most advanced hair transplant surgery cannot deliver long-term, natural results.
In this complete management guide, we will explore:
What the transplant donor area is
Why it is critical in hair restoration surgery
How grafts are removed from the donor
Differences between FUE and FUT donor management
Risks like overharvesting
Donor area healing and recovery
Long-term planning for progressive hair loss
Advanced cases including body hair extraction
Understanding donor area science is essential for protecting your hair for life.
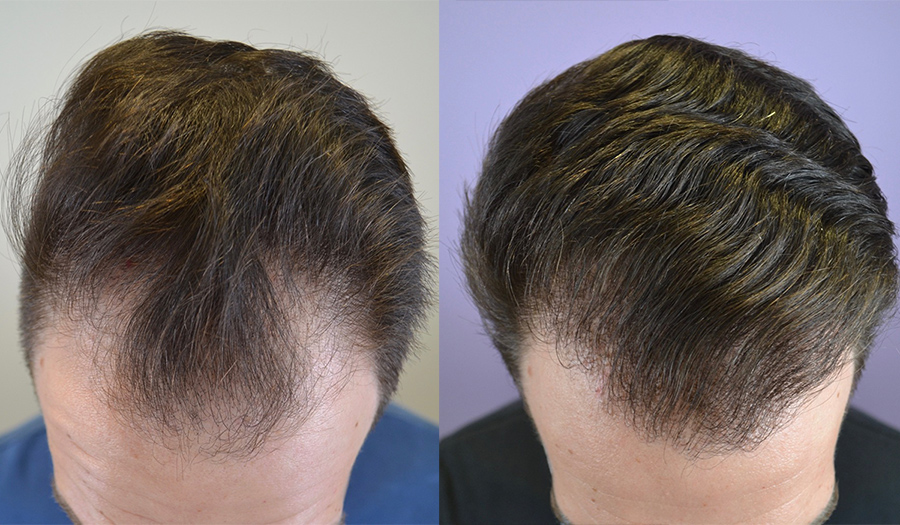
The hair transplant donor area is typically located on the back and sides of the scalp. These regions contain genetically resistant follicles that are less affected by male pattern baldness.
This is known as the “safe donor zone.”
Hair in this zone is resistant to DHT (dihydrotestosterone), the hormone responsible for most cases of hereditary hair loss. That’s why follicles from the donor can survive when moved to the recipient area.
Many patients obsess over the hairline design. But the reality is:
If the donor area is weak, the entire transplant strategy fails.
The donor determines:
Maximum graft capacity
Future transplant options
Long-term hair density
Natural balance
Sustainability of hair growth
A poor donor strategy can cause visible thinning at the back of the scalp — sometimes worse than the original baldness.
During a hair transplant procedure, grafts are removed from the donor and placed into the recipient site.
There are two primary extraction techniques:
Follicular unit extraction FUE involves:
Using a micro-punch tool
Extracting individual follicular units
Leaving tiny circular scars
Avoiding a linear scar
Each graft contains 1–4 hairs. These grafts are carefully harvested from the transplant donor area and implanted into thinning zones.
Advantages:
Minimal scarring
Faster recovery
No stitches
Natural-looking donor preservation when done correctly
Follicular unit transplantation FUT, also known as the strip method, involves:
Removing a strip of scalp from the donor site
Closing the area with sutures
Dissecting grafts under a microscope
This method leaves a linear scar but allows harvesting a large number of grafts in a single session.
FUT may be beneficial for:
Patients requiring high graft numbers
Individuals with tight donor capacity
Certain advanced cases of hair loss
However, modern trends favor FUE due to cosmetic flexibility.
The average scalp contains:
6,000–8,000 available grafts in the safe donor zone
Approximately 70–100 follicular units per cm²
However, not all follicles from the donor can be safely extracted.
Safe extraction rule:
Only 20–30% of hair density in a given area should be removed to prevent visible thinning.
Excessive extraction reduces hair density and may permanently damage the donor.
One of the most common mistakes in modern hair restoration surgery is overharvesting.
Overharvesting occurs when:
Too many grafts are removed from the donor
Extraction pattern is uneven
Density drops below natural camouflage levels
Results include:
Patchy appearance
Visible scarring
Thin back-of-head look
Cosmetic imbalance
An experienced hair transplant surgeon must distribute extraction evenly to protect donor aesthetics.
Healing depends on technique.
After FUE
Day 1–3: Tiny red extraction dots
Day 7–10: Scabs fall off
2–3 weeks: Surface healing
1–2 months: Full cosmetic blending
After FUT
10–14 days: Sutures removed
2–3 weeks: Linear scar closes
Several months: Scar softens
FUE offers faster visible recovery.
Temporary thinning in the donor site can occur, especially after large sessions.
Donor shock loss:
Usually temporary
Hair regrows within 3–6 months
Occurs more frequently in high extraction sessions
Proper surgical planning minimizes this risk.
The principle behind transplantation is called “donor dominance.”
Follicles from the donor maintain their genetic resistance to male pattern baldness even after relocation.
That means transplanted hair should continue natural hair growth long-term.
However, if donor selection is outside the safe zone, results may not be permanent.
Hair loss is progressive.
A responsible surgeon must plan for:
Future baldness expansion
Second or third sessions
Donor preservation
Long-term density balance
Removing too many grafts early reduces future options.
Strategic donor management is more important than aggressive single-session density.
A transplant is a redistribution of limited resources.
Every graft removed from the donor reduces hair density in that zone.
The surgeon must balance:
Donor strength
Recipient area coverage
Cosmetic harmony
A great hairline with a depleted donor is not a successful transplant.
In patients with weak scalp donor reserves, surgeons may consider body hair extraction.
Sources include:
Beard hair
Chest hair
Arm or leg hair (rarely ideal)
Beard hair is most commonly used because:
It is thicker
Growth cycle is strong
Density is higher
However, body hair behaves differently and requires expert planning.
In male pattern baldness, hair on the top of the scalp miniaturizes while the back and sides of the scalp remain stable.
However, in rare cases, donor thinning can occur.
Before surgery, a careful donor evaluation should assess:
Miniaturization percentage
Density per cm²
Hair caliber
Scalp elasticity
Not every patient is an ideal transplant candidate.
Patients should:
Avoid excessive short buzz cuts early
Protect scalp from sun exposure
Follow post-operative care
Avoid aggressive scratching
Maintain healthy nutrition
Long-term donor health supports future hair restoration options.
No.
Hair removed from the donor does not regrow in the same follicle.
This is why overharvesting is permanent.
Once follicles from the donor are removed, they are gone forever.
Proper planning protects donor longevity.
A strong transplant donor area has:
High hair density
Thick hair shafts
Stable DHT resistance
No diffuse thinning
Good scalp flexibility
These factors improve graft survival and overall hair growth in the recipient area.
Donor management depends heavily on the skill of the hair transplant surgeon.
Key competencies include:
Even extraction pattern
Correct punch size
Preserving surrounding follicles
Long-term strategic planning
Technique alone does not guarantee donor protection.
It determines:
Graft availability
Future procedures
Natural appearance
Long-term stability
Whether using follicular unit extraction FUE or follicular unit transplantation FUT, donor management must prioritize:
Preservation
Even extraction
Long-term planning
Avoiding overharvesting
A well-managed donor ensures healthy transplanted hair, stable hair growth, and lifelong aesthetic balance.
The best transplant is not the one that uses the most grafts — it’s the one that respects the donor.